Featured Survivor Story:
Survivor Spotlight: Acral Melanoma Survivor

Melanoma Can Hide in the Most Unlikely Places
By Mara Klecker
Lisa first noticed a pale band on her right big toenail about a decade ago, when she was pregnant with her son. She brought it up to her dermatologist at the time, and he said to keep an eye on it, but he wasn’t too concerned. He suspected it was a mole that had darkened with the hormones of pregnancy.
Then, last August, Lisa rubbed off the nail polish she’d had on her toenails for a few months. Underneath, she saw that the band had gotten much darker.
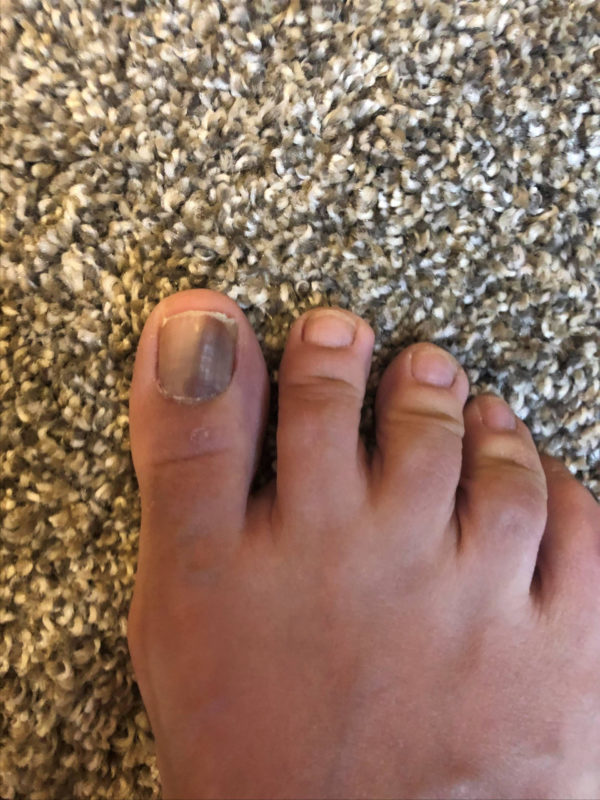
August 2020: Darkened streak on the right big toenail
Lisa works in medical education and has an extensive network of contacts with dermatology and oncology expertise. She knew immediately that she should have someone look at the darkened band because it was a sudden change. But the next appointment with her dermatologist wasn’t for another two and a half months.
So she sent a photo of her foot to a friend, who is a dermatopathologist. That friend recommended she push her dermatologist appointment up.
“The great thing is that I pretty immediately had people helping me with this,” Lisa said.
Once she explained the sudden darkening of the band, her dermatologist told her to come in right away. Lisa had been in just a few months earlier for her annual full-body skin check, but she hadn’t taken her socks off.
“That’s one pearl of wisdom I learned: Insist that your provider look at your hands and feet when you go in for a skin check,” she said.
Once the dermatologist saw Lisa’s toe, she scheduled a nail matrix biopsy. At the end of August, just a couple of days after her appointment, Lisa underwent the procedure, which involved taking a tissue specimen from the area of the toe that produces the nail plate as well as half of her toenail.
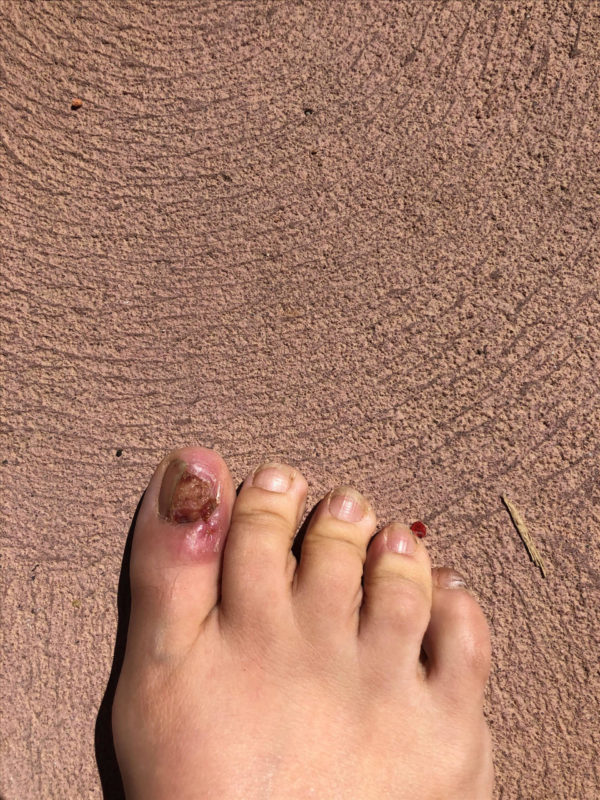
September 2020: Post biopsy. Note that half of the nail plate was sent for pathology and there you can see the remnants of the stitch where they peeled the skin back to access the nail matrix for the biopsy.
The biopsy results showed that Lisa had an early in situ nail matrix melanoma. At this point, Lisa contacted AIM at Melanoma, and their staff helped her evaluate the options that her dermatologist presented.
Lisa opted for modified Mohs surgery to remove the melanoma. In this procedure, the Mohs surgeon first took out the whole nail matrix and nail and sent it for regular pathologic assessment. Then the surgeon took a 6 mm margin of skin and evaluated it in the office. This is the advantage of the Mohs procedure: It allows the surgeon to look immediately and decide if there is any cancer left and whether they need a second round of excision. Lisa was very pleased that when the pathology from the nail matrix portion came back, she did not have any tumor left after the biopsy.
But the surgery removed her entire toenail and required a skin graft from Lisa’s underarm.
“It was a long recovery of a couple months,” Lisa said. She wore Velcro sandals over socks because her foot couldn’t slide into most shoes.
Lisa had a prescheduled trip, so, she used a wheelchair and had to be extra careful that no one bumped into her healing toe – something she was extra cautious about at the airport.
“You never really think about having to protect your toe,” she said. “But it was so important to make sure the skin graft healed.”
She also used a cut-off stocking to make a tube that could go over the bandages and keep them in place on the skin graft donor site so she could avoid the tape that irritated her skin.
But the recovery wasn’t all just about managing the physical wounds.
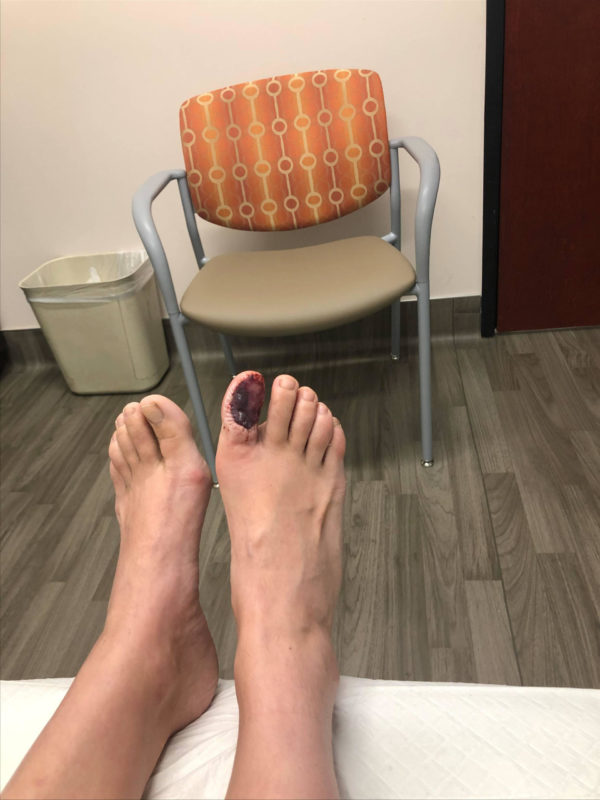
October 7th. Wound check 2 days post surgery showing the surgical site with the skin graft sutured in place.
“Part of it was also dealing with the mental side of it all,” Lisa said. “It’s a major trauma to go through a cancer diagnosis.”
Now, more than six months after her surgery, Lisa says she still carries a “baseline anxiety” about the cancer returning. But she’s grateful for what the diagnosis helped her realize.
“You come back with perspective,” she said. “You realize ‘I just faced cancer, so I shouldn’t be upset about the little things.’”
Instead, she’s learned to notice those smaller moments and be grateful for them. The recovery process forced her to slow down and let others help her and her family.
“You might not want to tell the whole world that you have cancer, but if you tell the right people, they’ll want to help you,” she said. “And I learned that it’s OK to be on the receiving end of that care and help.”
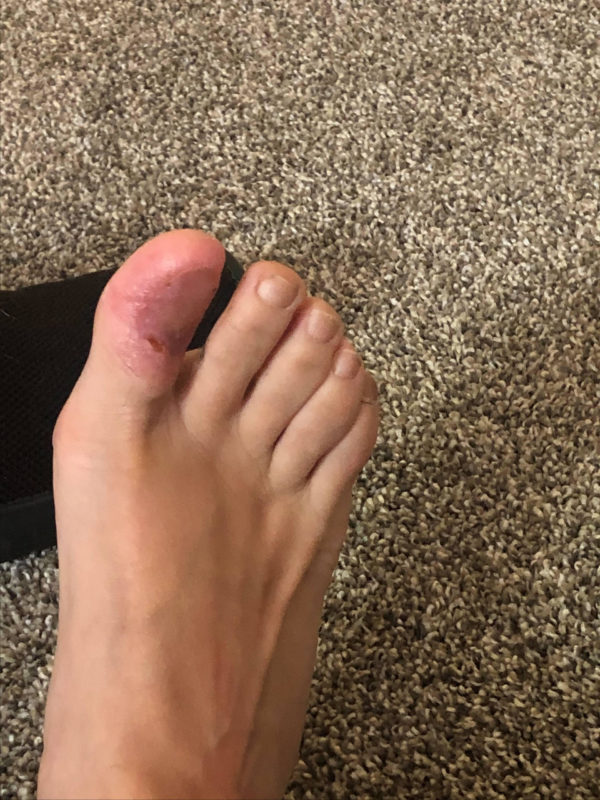
Almost healed approximately 6 weeks post surgery.
Lisa also has other “pearls of wisdom” from her melanoma experience:
- Everyone, not just fair-skinned people, needs to be aware of skin cancer and its signs. Though melanoma of the nail unit is rare, it can occur in people of all races.
- When visiting the dermatologist for an annual exam, make sure your doctor looks at your feet and hands. And remove any nail polish.
- Don’t write off a dark band in a fingernail or toenail as simply as a hemorrhage from injury. Melanoma of the nail unit can often present as a pigmented band. It can also cause cracking of the nail plate.
- If you do have a concern about your nail, find a dermatologist with expertise in nail matrix biopsies.
Lisa said even with her extensive network and her access to information about melanoma, she found it challenging to process the diagnosis and sift through the varied perspectives on her condition.
“That’s the reason we need places like AIM at Melanoma,” she said. “Reliable patient education is so important.”
Recent Posts

Fifth Annual Evening in Memory of Valerie Guild

Results for darovasertib in combination with crizotinib in first line HLA*A2:01-negative metastatic uveal melanoma met the study’s primary objective

Encouraging results with anzutresgene autoleucel in patients with uveal melanoma and other melanoma subtypes

Promising early results with imneskibart, low-dose subcutaneous IL-2, and nivolumab in patients who do not respond to or who relapse after receiving combination checkpoint inhibitors


