Other Skin Cancers

What Are The Other Types of Skin Cancers?
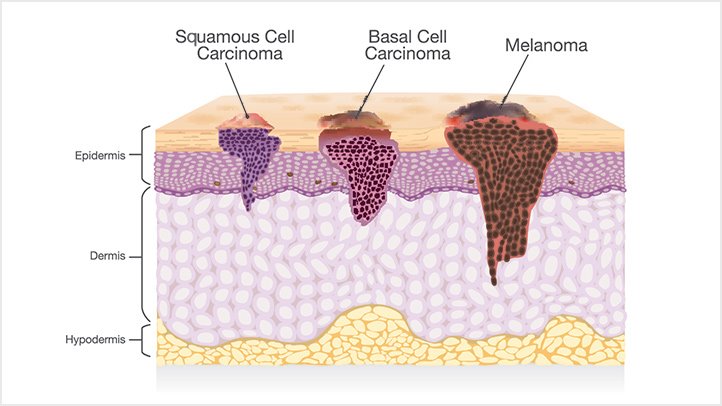
Skin has two distinct layers: the epidermis , which is on the outside, and the dermis , which is underneath the epidermis. These two layers are made up of millions upon millions of cells, four of which are directly related to skin cancer.
Squamous cells reside on the skin’s surface—the top of the epidermis— and are constantly shed as new ones form. Basal cells reside in the lower part of the epidermis, called the basal cell layer. Basal cells divide and move up through the epidermis to replace the lost squamous cells and become squamous cells themselves in the process. Merkel cells are found at the base of the epidermis and they help us sense touch. Melanocytes, also found at the base of the epidermis, are cells that produce melanin, the pigment responsible for coloring our skin.
Skin cancer is an abnormal growth of skin cells. When any of these types of cells become damaged, they may develop into skin cancer. It most often develops on areas of the skin exposed to ultraviolet (UV) light. Skin cancer affects people of all colors and races, although those with lighter skin who sunburn easily are at higher risk for developing skin cancer.
All skin cancers are dangerous and should be treated promptly. But prognoses and treatment options vary widely depending on the types of cells affected. Melanoma develops in the melanocytes and is the deadliest type of skin cancer. The rest of this website is devoted to melanoma. Three other types of skin cancers are discussed here: basal cell carcinoma (BCC), cutaneous squamous squamous cell carcinoma (cSCC), and Merkel cell carcinoma (MCC). The first two skin cancers are often grouped together as non-melanoma skin cancers. Left untreated, these skin cancers can spread to other organs and become fatal.
Basal Cell Carcinoma (BCC)
- Over four million cases of basal cell carcinoma are diagnosed in the United States each year, making it not only the most common form of skin cancer but the most common form of any type of cancer.
- This cancer develops in the basal cells of the skin, which are found at the base of the epidermis (the outer skin layer). Basal cell carcinoma usually occurs in the areas of the skin that receive the most exposure to the sun—the head and neck—but can develop on other areas of the body, including the genitals.
- BCC usually grows slowly, and while it is very rare for it to spread, or metastasize, to nearby lymph nodes or more distant parts of the body, spreading may occur if it is left untreated. The spread can be disfiguring. As with all skin cancers, early detection and treatment are important.
- The appearance of basal cell carcinomas can vary widely, including but not limited to a small, shiny bump or nodule on the skin; an area of thickened skin or a red patch; and an open sore that doesn’t heal.
- Patients who have had one basal cell carcinoma have an increased risk of developing a new BCC elsewhere. Forty to 50 percent of these patients will develop a new BCC within five years of their first diagnosis.
Cutaneous Squamous Cell Carcinoma (cSCC)
- Cutaneous squamous cell carcinoma is the second most common type of skin cancer, accounting for approximately 20% of all non-melanoma skin cancers. It develops from squamous cells that make up much of the surface of the epidermis.
- More than 1 million cases of cutaneous squamous cell carcinoma are diagnosed in the U.S. each year.
- Middle-aged and elderly people are most likely to develop cSCC, especially those with light-colored skin and a history of frequent UV exposure.
- This skin cancer often appears as a bump or nodule, or as a red, scaly patch on the face, lips, mouth, or ear.
- cSCC often arises from small, scaly growths on the skin called actinic keratoses (see below for more on actinic keratoses). A cSCC can occur anywhere on the body because squamous cells exist on every part of our skin, even the skin inside our mouths.
- cSCC is more likely than BCC to metastasize and spread to other areas of the body if not treated in a timely manner, so early detection and treatment of cSCC is critical.
Merkel Cell Carcinoma (MCC)
- Merkel cell carcinoma is a rare but aggressive form of skin cancer.
- It begins in Merkel cells, which are found in the base of the epidermis.
- MCC usually appears as a red, painless lump in sun-exposed areas such as the neck, face, or head.
- People over 50 with a compromised immune system are at higher risk of developing this type of skin cancer. Merkel cell carcinoma tends to grow rapidly and spread quickly to other parts of the body. Treatment options for MCC depend on whether it has spread.
Other Cancers and Pre-Cancers That Appear on the Skin
Actinic Keratosis (AK) is a common pre-cancerous growth that may develop into squamous cell carcinoma if left untreated. This growth appears as a rough, scaly patch on your skin that may be pink-red or flesh colored and develops from years of exposure to the sun. It’s most commonly found on the face, lips, ears, back of the hands, forearms, scalp, or neck.
Keratoacanthoma (KA) is a low-grade, slow growing and typically benign tumor that looks like a tiny dome or crater. Keratoacanthoma originates in the skin’s and often goes away on its own. KA is considered by some to be a highly differentiated form of squamous cell carcinoma.
Kaposi Sarcoma (KS) KS is not a skin cancer but a cancer that can appear on the skin or on mucosal surfaces. The lesions or tumors are often brownish-red to purple or blue in color and usually found on the legs, feet and face. This cancer is caused by a type of herpes virus, typically in patients with weakened immune systems, such as those with AIDS.
Lymphoma of the Skin, or Cutaneous Lymphoma, is a rare type of non-Hodgkin lymphoma that can appear as a rash or bumps on the skin. Most cases of lymphoma form in the lymph nodes, but lymphomas may also develop in other lymphoid tissue, including the spleen, bone marrow, and skin.
Be Proactive
The quicker skin cancer is detected, the better the long-term outlook. Check your skin regularly. If you notice abnormalities, consult a healthcare provider for a complete examination. Learn how toself-examineyour skin. Preventive measures, such as wearing sunscreen, wearing sun-protective clothing, limiting your time in the sun, and avoiding tanning beds and other tanning devices, are your best protection against all types of skin cancer.
For comprehensive information about non-melanoma skin cancers, visit our website, AIM at Skin Cancer. This invaluable resource is designed to equip you with essential knowledge and practical tools, helping you gain a deeper understanding of non-melanoma skin cancers.

