Skin Lesions That May Become Melanoma
Two types of pigmented lesions are associated with an increased risk of developing melanoma: congenital nevi and atypical nevi.
Congenital Nevi
A congenital nevus, also known as a mole, is a type of pigmented birthmark that appears at birth or during a baby’s first year. These occur in 1-2 percent of the population. These moles are frequently found on the trunk or limbs, although they can appear anywhere on the body. Congenital nevi are thought to be caused by a genetic mutation, called a sporadic mutation, which develops randomly as a baby grows in the womb. The condition is not inherited.
Congenital nevi (the plural of nevus) can be skin-colored, tan or brown. They can be flat or raised, and small or large. They may or may not have hair growing from them when they first appear, but can also develop hair over time.
Most congenital nevi usually do not cause health problems, but a small percentage may develop into melanoma later in life. The risk of melanoma increases with the size of the nevus.
A rare form of congenital mole is the large congenital melanocytic nevus (LCMN), which occurs in approximately 1 in 20,000 newborns worldwide. It is present from birth (congenital) or is noticeable soon after birth. The nevus may be small in infants, but it will usually grow at the same rate the body grows and will eventually be at least 40 cm (15.75 inches) across.
These moles have the greatest risk of developing melanoma.
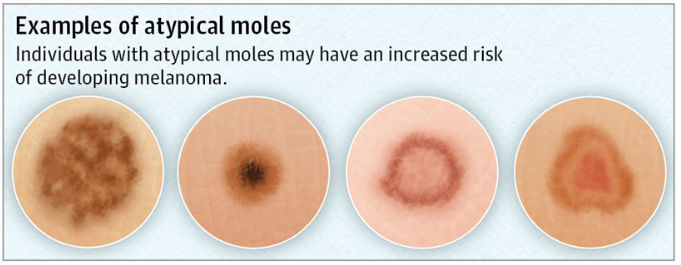
Atypical Nevi (dysplastic nevi)
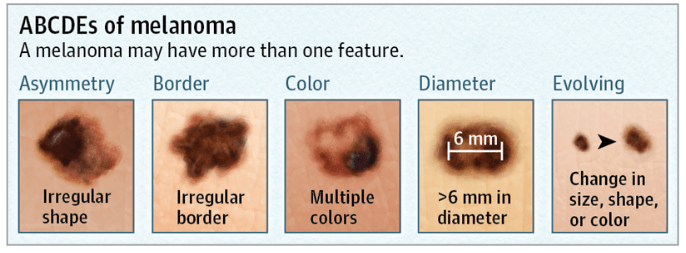
Atypical moles, also called dysplastic moles, are very common. These moles are larger than common moles, with borders that are irregular and poorly defined. Atypical moles also vary in color, ranging from tan to dark brown shades on a pink background. They have irregular borders that may include notches. They may fade into surrounding skin and include a flat portion level with the skin. Sometimes they are described as looking like fried eggs, with a raised center of darker pigmentation surrounded by a flat, lighter area. Atypical nevi may occur anywhere on the body, but are found most frequently on the back and on sun-exposed areas. People with many atypical moles, or who have relatives who have had melanoma, may be at greater risk for melanoma.
Tips for Self-Monitoring and Prevention
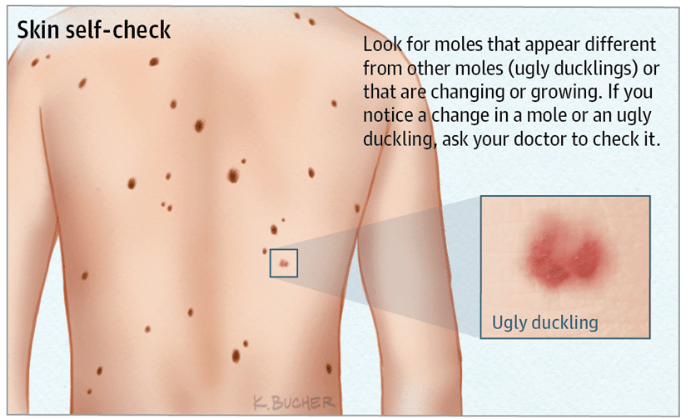
If you have atypical moles, you should do a skin self-check on a monthly basis. Your doctor should check any moles that suddenly change in size or color or that persistently itch or bleed. In addition, if you have a spot on your skin that does not look like any of your moles (an “ugly duckling”), you should ask your doctor about it. Excessive sun exposure (or tanning bed use) increases your risk for melanoma. Protect yourself by covering up with sun-protective clothing and hats. Wear sunscreen (SPF 30 or greater) on sun-exposed skin, and minimize the time you spend outdoors when the sun is strongest, between 10:00 am and 2:00 pm.